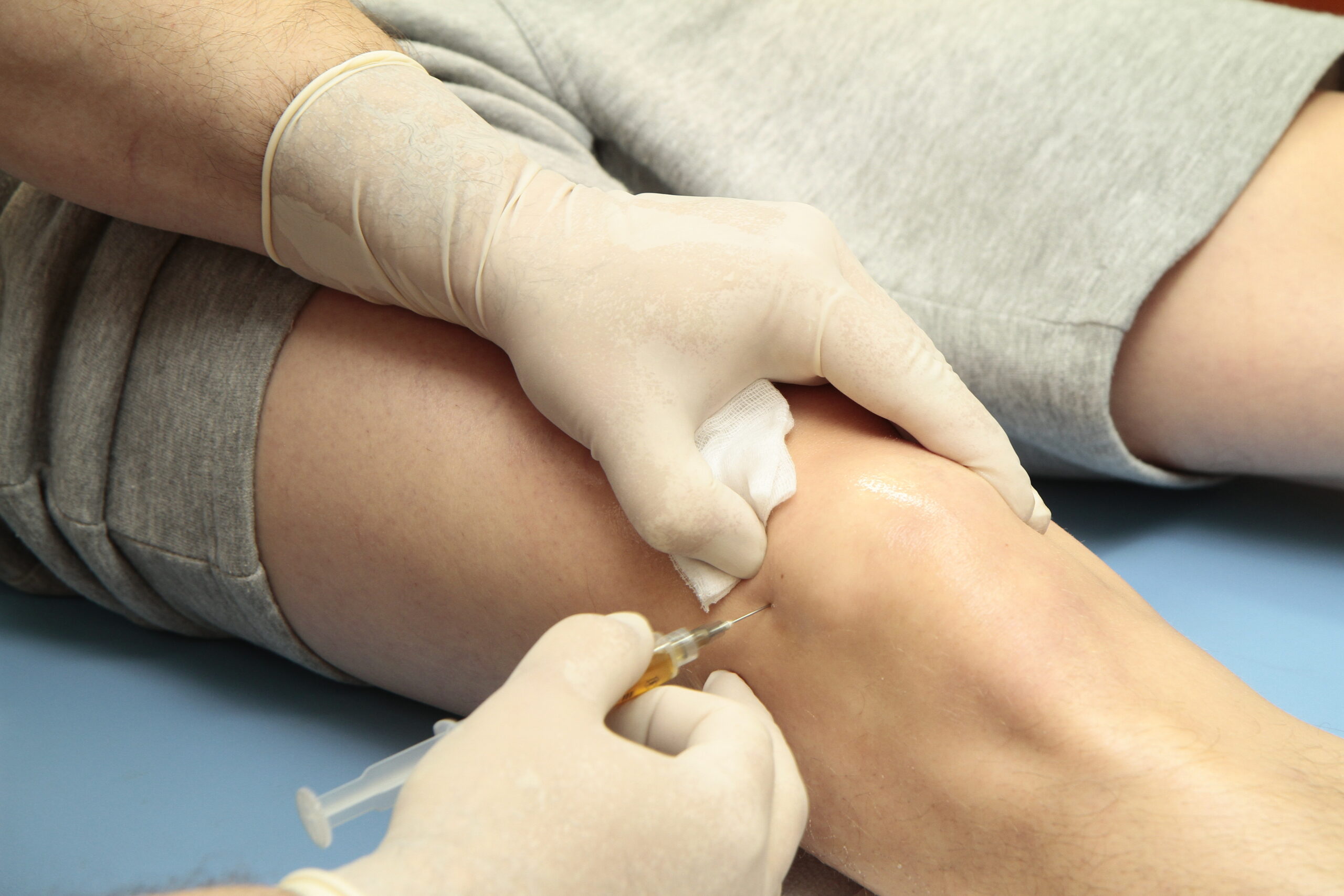
Is Platelet Rich Plasma Therapy For You?
Have you ever had a persistent injury that’s taking longer to heal than expected? Maybe those stretches you saw on Instagram or TikTok just aren’t doing the trick, or maybe your attempts with physical therapy just can’t clear up that stubborn painful area in your body yet. Whatever the case may be, platelet rich plasma therapy might be the solution for you! This blog post will run through what platelet rich plasma is, which injuries the current evidence supports the use of platelet rich plasma for, and what recovery is like after the injection.
What is PRP Therapy/Injection?

Platelet-rich plasma therapy or PRP for short, is a form of regenerative therapy that uses your own body’s natural growth factors to heal tissues. PRP therapy utilizes your own blood that has been spun to separate the other parts of your blood from nutrient-rich platelets, which are then injected directly into an injured tissue to stimulate increased growth factors and the amount of reparative cells (in other words, more of the good stuff to heal your injury faster). PRP therapy, in theory, has the ability to heal damaged tissues as opposed to traditional medical approaches that simply mask the pain associated with damaged tissue.
When is it used?
Initially established and used for dentistry, dermatology, plastic/maxillofacial surgery, acute trauma, cosmetic surgery, and veterinary medicine, PRP has transitioned into the orthopedic world for its potential healing qualities for a variety of tissue types. If you’re reading this blog, you’re likely curious about PRP therapy for a targeted musculoskeletal purpose. Because the application of PRP for musculoskeletal injuries is still a relatively novel concept, limited data to support the effectiveness of PRP interventions are available. Below is a brief summary of the available research for different types of musculoskeletal injuries.
Tendinopathies1
There is some clinical evidence to support PRP injections for tendinopathies. Specifically, in a study by Mishra and Pavelko et al., 93% participants reported a reduction in epicondylar (elbow) pain at a 2-year follow up after receiving a single PRP injection. Another study by Kon et al. cited significant improvements in quality of life, pain, and sporting activity after 6 months for those that received 3 PRP injections at 15-day intervals for 20 participants with patellar tendinosis (the tendon under the kneecap). If at this point PRP sounds to you (and your painful tendons) like the best thing since sliced bread, it doesn’t always prove to be the case. A recent randomized control trial (RCT) concluded that PRP injections for chronic achilles tendinopathy did not improve patient pain or activity compared to a saline injection control. In other words, according to Vos et al.’s randomized control trial, PRP fared no better than a placebo injection. Other uses of PRP for tendinopathies include the shoulder rotator cuff. While there is conflicting evidence supporting PRP for rotator cuff tendinopathies, it may be something to consider in combination with shoulder rotator cuff surgical repairs.
Ligament Injuries1
The utilization of PRP injections to accelerate ligament injuries appears to be more controversial and conflicting. Studies have cited the use of PRP therapy for anterior cruciate ligament (ACL) and medial collateral ligament (MCL) injuries with some studies reporting increased tendon tensile strength and improved healing times, while others reporting no significant changes in the mechanical properties of healed tendons in animal studies.
Muscle Strain Injuries1
PRP is not commonly used for muscle strain injuries and there are currently no human clinical studies investigating the efficacy for PRP therapy in muscular injuries to date.
Cartilage Injuries, Osteoarthritis (Early)1, 2
Articular cartilage inherently has poor regenerative capacities making treatment for articular disease, such as osteoarthritis, a challenge in the world of orthopedics. A clinical study of 100 patients diagnosed with degenerative cartilage lesions of the knee that used PRP therapy indicated that PRP injections are safe and show the potential to reduce pain, improve knee function and quality of life in young patients with low degrees of articular degeneration. Research also cites the positive effects of PRP for early osteoarthritis. However, the benefits appear to wear off after 6-12 months. More robust randomized controlled studies will be critical to confirm the true potential of PRP for treatment of cartilage degeneration.
Is PRP therapy for you?
It depends! Based on the current research findings, evidence supporting the positive effects of PRP are encouraging for some injuries, but not conclusive and definitive. More often than not, PRP injections should not be the go-to option for tissue healing at this time and other interventional approaches should be trialed first. In addition, most medical insurance plans do not cover PRP injections. According to the UW Family Medicine website, PRP injections cost $600-900 out of pocket depending on the concurrent use of ultrasound or not.4 Elsewhere, PRP injections have been noted to cost an upwards of around $2000 per session. However, if you’ve exhausted other means of rehabilitating and/or managing your specific injury, you should consider consulting a PRP or regenerative medicine specialist.
The current research most strongly supports the use of PRP therapy for lateral epicondylitis (tennis elbow) with symptoms that persist more than 3 months and early knee osteoarthritis if corticosteroid injections/hyaluronic acid attempts have not been effective.3 It should also be considered for the elite athlete with high ankle sprains5 (Samra et al.) or refractory patellar (knee cap) tendinopathy.3
What is recovery like?3
Rehabilitation after PRP therapy has not been standardized at this time but typical post-operative principles are applied. An abbreviated post-operative protocol may be assigned after PRP therapy. Early stages (0-5 days) aim to protect the injected area by avoiding placing excessive stress and strain through the tendon or joint. Later stage rehab will focus on reintroducing normal stress and strain through the injected tissue to restore normal tissue capacity.3 The highly trained physical therapists at MTI Physical Therapy can help you rehabilitate your injury. They will assess your unique situation and create a treatment plan tailored to address your needs and help you get back to the activities you love. Contact us and get started today!
Key Points
- Platelet rich plasma injections use your own blood that is concentrated and injected into an injured bodily tissue to accelerate the healing process
- Based on the current research, it is most effective for:
- Tennis/golfers elbow (medial/lateral epicondylalgia)
- Degenerative cartilage lesions of the knee/early knee osteoarthritis
- Elite athletes with high ankle sprain5
- Refractory patellar (kneecap) tendinopathy
- Recovery after PRP injections are not standardized, but a post-operative protocol may be prescribed to you and administered by your physical therapist
Citations:
- Cole, Brian J et al. “Platelet-rich plasma: where are we now and where are we going?.” Sports health vol. 2,3 (2010): 203-10. doi:10.1177/1941738110366385
- Kon, Elizaveta, et al. “Platelet-Rich Plasma: Intra-Articular Knee Injections Produced Favorable Results on Degenerative Cartilage Lesions.” Knee Surgery, Sports Traumatology, Arthroscopy, vol. 18, no. 4, 2009, pp. 472–479., https://doi.org/10.1007/s00167-009-0940-8.
- Kristen Wingfield, et al. “PRP: What happens after the injection?” UCSF Medical Center, https://orthosurgery.ucsf.edu/sites/default/files/2021-08/PRP-2021-KWpdf.pdf
- “Regenerative Medicine.” UW Department of Family Medicine, https://familymedicine.uw.edu/sports-medicine/patients/regenerative-medicine/#:~:text=PRP%20is%20not%20covered%20by,in%20all%20joints%20except%20knees.
- Samra, D., et al. “Effectiveness of a Single Platelet Rich Plasma (PRP) Injection to Promote Recovery in Rugby Players with Ankle Syndesmosis Injury.” Journal of Science and Medicine in Sport, vol. 19, 2015, https://doi.org/10.1016/j.jsams.2015.12.496.